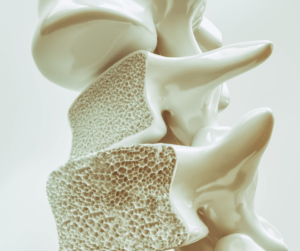
Why think about your bone health? Bone is living tissue that is constantly being broken down and replaced. Yet the way your body replaces your bone tissue can change and diminish. Osteoporosis is disease in which the creation of new bone doesn’t keep up with the loss of old bone. Women who are past menopause are at highest risk. However, men may develop osteoporosis as well.
Osteoporosis is a sneaky disease. It is essentially painless. You may not know you have osteoporosis until after you break a bone. As this health issue advances, one can end up with surprisingly painful fractures and bone deformities. As the disease weakens the bones, injuries, such as a minor bump or fall, can lead to loss of the quality and the quantity of your life. can lead to loss of the quality and the quantity of your life.
According to the International Osteoporosis Foundation, osteoporosis a affects over 200 million people world wide. According to the National Osteoporosis Foundation approximately 10 million Americans have osteoporosis and another 40 million have low bone density. One in two woman and one in four men will break a bone and a lifetime due to osteoporosis.
“Osteoporosis is a silent disease,” says Dr. Edith Cullen, a musculoskeletal physician and osteoporosis specialist at the Orthopedic & Sports Medicine Center (OSMC). She continues, “You cannot feel your bones getting weaker. Ironically, your greatest opportunity for prevention was when you were in your teens and twenties when your diet and exercise habits helped build strong bones.
Not sure you did your part for your bones in your earlier years?
Don’t throw in the towel yet! At any age, there are many things you can do to protect your Bone Health and decrease your risk of painful broken bones. The first step is to talk to your healthcare provider.
Dr. Cullen says that there are steps you can take to protect yourself, no matter your age. “You can improve your bone health. Start by getting the appropriate calcium and vitamin-D daily. Do regular weight-bearing and muscle strengthening exercises. Do not smoke or drink too much alcohol. Also talk to your provider about yuour chance of getting osteoporosis and when you should have a bone density test,” she says. A bone density test helps to show the strength and thickness (known as bone density or mass) of your bones. It is called a DEXA Scan, which is a low-dose x-ray scan that allows a doctor to identify when bone loss is occurring before you suffer a fracture. Certain medications, lifestyle, and nutrients may then be suggested to help to slow the rate of bone loss.

Sources of Osteoporosis Fracture Pain
The risk of a fracture, or broken bone, increases as your bones lose mass. Before osteoporosis sets in, a mishap like tripping and falling from a low height may have only caused a bruise. But when you have osteoporosis, that same fall can cause serious damage and even increase your chances of premature death. “My mother, who is in her 80’s has been diagnosed with osteoporosis, gently slipped off the couch to the floor. She ended up with six painful cracks in the back of her pelvis. The orthopedic surgeon placed six metal rods in the area to secure her from further damage,” commented Paige Mayers from South Bend.
The most common sources of pain include:
- Micro trabecular fractures. These are tiny cracks in the bone.
- Compression fractures. These fractures are compressions of the bony vertebral bodies in the spine. Compression fracture deformities can cause pain, problems with eating, breathing, mobility, and balance.
- Nerve pain. Fractures of a vertebra from osteoporosis can compress a nerve, which can cause pain.
- Stress Fractures. These fractures occur during routine daily tasks or activities without traumatic injury.
- Low Trauma Fractures. These occur with low trauma, such as a fall or other injury that would not ordinarily cause a fracture. These fractures may include a broken hip, pelvis, arm, wrist, or leg.
Managing Osteoporosis Fracture Pain
“An Osteoporosis diagnosis is not necessarily a promise that you will have a bone break and have to live with constant pain,” notes Dr. Cullen. “There are several solutions available, and your overall health will dictate your best options for your osteoporosis management.”
The following solutions are most common when treating osteoporosis:
- Rest and rehab. Taking it easy may give your body some time to heal after an injury.
- Physical therapy. The therapist will more-than-likely develop a routine specifically for osteoporosis to improve strength and balance.
- Medication. Your doctor may recommend diet, exercise, osteoporosis medication and bone-healthy vitamins and minerals.
- Assistive Devices. Customized brace, cane, walker, and other assistive devices for walking or other motions can help with pain, bone healing and fall prevention.
Weak bones can be addressed. See your healthcare provider and ask them what type of screening schedule might be right for you. It will depend on your age and risk factors for the disease.
Book an appointment easily, online, with Dr. Cullen or call 574-264-0791.
This blog post is not intended to provide personal medical advice, professional diagnosis, opinion, treatment to you or to any other individual. It is information for educational purposes only. You should not use this information in place of a consultation or the advice of a healthcare provider.



